With Covid-19 cases increasing, France’s National Academy of Medicine has called for the mandatory vaccination of care providers against the seasonal flu to avoid comprising the health care system, raising a debate about medical ethics.
The Covid-19 pandemic, which risks returning to epidemic proportions in France in the autumn and winter months, means public authorities should reconsider whether to make vaccines mandatory for health workers, the academy said in a communiqué on Saturday.
“It is urgent to make the flu vaccine mandatory for all health care personnel,” said the academy, a learned society that advises the government on matters pertaining to medicine, disease, and public health.


Read also: Agyapa Royalties Deal; Exactly What Dr. Nkrumah Was Fighting Against – Ivor Greenstreet
“The current evolution of epidemiological indicators raises fears of the persistent circulation of SARS-CoV-2 at epidemic levels until next spring,” meaning “the risk of a saturation of hospital services with the addition of severe flu cases on top of Covid-19 cases, exacerbated by the incapacity of sick staff, cannot be risked.”
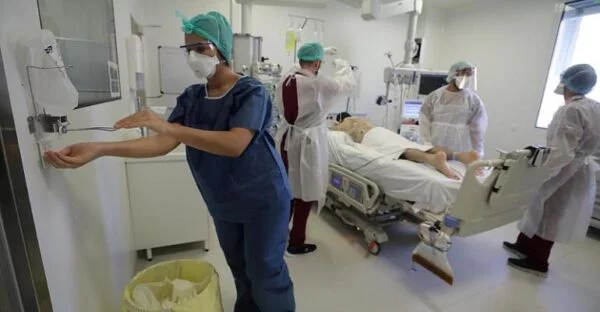
Health experts fear that an epidemic of the flu, which has killed 8000 to 14,500 people in France per year for the past three years, could increase strain on intensive care units occupied by COVID patients.
Care providers get vaccine less than average
France’s campaign for the seasonal flu vaccine targets groups most vulnerable to complications in the event of a flu infection, including the elderly, people with pre-existing medical conditions, and pregnant women.
Some 45 percent of the population gets the flu shot in an average year, and although the vaccine is strongly recommended, participation is lower among health care staff than the overall average.
Citing health agency figures, the academy said an estimated 35 percent of hospital care staff participated in the flu vaccine campaign in 2018-2019, including 67 percent of doctors, 48 percent of midwives, 36 percent of nurses, and 21 percent of assistant nurses.
In care homes for the elderly, the overall figure was slightly lower at 32 percent, including 75 percent of doctors, 43 percent of nurses, 27 percent of assistant nurses, and 34 percent of paramedical staff.
“Vaccination among health care personnel against the seasonal flu remains insufficient,” the academy said.
Ethical debate
In general, each country decides whether to make vaccines voluntary or compulsory, and for which populations. Some academy members even recommended extending compulsory vaccines beyond care providers.
“It must be made mandatory for people over 65 and for care providers,” former health minister and current academy president Jean-François Mattéi told newspaper Le Parisien.
The flu vaccine tends to be voluntary because it provides individual protection for one season. It is never 100 percent effective, and its effectiveness varies from one season to the next, since it is based on predictions of mutations that are sometimes wrong or imprecise.
“In terms of individual protection, one has the right risk catching the flu instead of getting the vaccine. It’s an individual liberty,” says Daniel Floret, vice-president of the vaccines technical commission with the HAS, a high authority advising the government on public health matters.
The academy argues that the duties of health care professionals to protect and to be available for patients creates an ethical obligation for them to get the vaccine, a view shared by some doctors.
“For health care professionals, there’s another dimension,” says Serge Gilberg, a general practitioner and professor of at Paris-Descartes University medical faculty specialising in vaccines.
“They risk infecting their patients, and if they have the flu, they cannot work, which could leave health services short-handed at a moment that professionals are needed. So I would not find it shocking if the flu vaccine was mandatory for health care staff, but not for the general population.”
To date, no public officials have indicated the flu vaccine would be mandatory, and the government has not solicited the HAS for a recommendation on the matter.



